What is radiotherapy?
Radiotherapy uses carefully calculated and measured doses of radiation to treat cancer, as well as some non-malignant conditions. It affects all cells in the area being treated – preventing them from growing and dividing. The aim is to destroy as many abnormal (cancer) cells as possible. Some normal cells will be affected but they can usually repair the damage. The treatment is painless and only takes a few minutes.
It’s used to:
Attempt to cure cancer (radical radiotherapy)
Control/slow down the growth of cancer
Relieve cancer symptoms (palliative radiotherapy)
External beam radiotherapy delivers radiation from outside the body. Brachytherapy delivers radiation to body cavities or tissues internally using a specialist machine.
Radiotherapy can be used alone or with surgery, chemotherapy, or both. Your doctor will explain why radiotherapy has been recommended for you, and what you can expect.
Like any other form of treatment, radiotherapy has risks as well as benefits. The risks relate to the organs and tissues that receive treatment. You may experience temporary side effects such as discomfort, pain, or disruption in normal functions, for example changes in bowel habits if your abdomen (tummy) or pelvis is treated. These effects are predictable and can be managed with medicines, other therapies and support from staff. The effects usually settle within a few weeks after radiotherapy is completed.
There is a small risk of long-term damage, but this depends on many factors. The severity and possible impact on your life will be discussed with you and any risks will be weighed against your current health needs.
Radiotherapy at The Clatterbridge Cancer Centre
Our modern radiotherapy facilities include linear accelerators, superficial and orthovoltage X-ray treatment machines, simulators, scanners and 3D planning systems. The Trust also contains the National Centre for Eye Proton Therapy – the only centre in the UK offering this treatment for eye tumours.
We can offer both standard and specialised radiotherapy treatments. These include:
Treatment of prostate cancer
Total Body Irradiation
Total body electron therapy for widespread skin cancer
Intensity Modulated Radiotherapy
Papillon radiotherapy
Stereotactic radiosurgery
Rapid arc radiotherapy
Our staff work in lots of different areas of Radiotherapy, from the Physics department - who are responsible for the commissioning, maintenance and quality assurance of equipment - to the radiographers, assistant practitioners and Healthcare Support Workers, who look after the clinical and technical needs of our patients during treatment.
Attending the radiotherapy department
If you have any special needs or requirements please let the department at the site at which you are being treated know in advance so we can offer assistance.
We can book transport for patients who are on Radiotherapy treatment via the following providers:
North West Ambulance: 0800 032 3240
West Midlands Ambulance: 0345 425 0050
Welsh Ambulance Service: 0300 123 2303
You should eat and drink normally before your treatment. If you are on regular medication, please bring enough to cover your travel and treatment time.
Pregnancy and radiotherapy
Please note that before planning and treatment, women of childbearing age (12-55 years old) will be asked if they could be pregnant. This may seem insensitive, but the law requires radiographic staff to exclude this possibility before any procedure, which uses radiation for either diagnosis or treatment. The regulations are designed to protect the unborn child.
You will be asked to sign a form to show that this subject has been discussed.
If you are in any doubt about the possibility of being pregnant, please discuss this with your radiographers before undergoing any procedure involving radiation.
Radiotherapy planning
We need to find out about the shape and size of the area of the body to be treated and then match it against images and reports from previous scans, knowledge of the disease process, and reports at the time of surgery. This information is then used to design an individual treatment map, perform a dose calculation and finally, allow a radiotherapy treatment prescription to be written.
There are different types of equipment and procedures. Some are quite simple and require the doctor to mark the treatment area on the skin, while others are more complex, requiring a CT scan (CT planning). A small number of patients may also need to have a planning MRI or PET scan.
The average appointment time for a planning procedure is approximately 30 minutes per procedure/scan.
Preparation for planning
If your procedure requires any special preparation it will be discussed with you by the doctor from the Oncology team and again by the radiographers when you attend. A few patients will require an injection of a contrast agent (IV contrast), which can cause a mild reaction, such as a hot flush. If you have an IV injection as part of your planning process we will ask you to remain in the department for 30 minutes after the injection.
If you are having radiotherapy to the abdomen (tummy) or pelvis, you may need to drink some liquid before the scan (oral contrast). This liquid makes the bowel appear white on the scan pictures, which helps it stand out from other structures.
What to expect during radiotherapy planning
When you enter the hospital, there will usually be a volunteer or member of staff who can help you with directions and any other queries.
When you arrive at the planning department a radiographer will explain the procedure and answer any questions.
You will be monitored throughout the procedure but don’t worry if staff don’t talk to you, as they will be concentrating on the technical aspect of the process. Your consultant may not be present for some, or all of your procedure as their input is needed later in the process, but it is still their responsibility to ensure that appropriate planning procedures have been undertaken.
We’ll also need to make a few small marks on your skin using a felt tip pen. These will be made permanent at the end of the process, with your permission, by tattooing a small dot. We do recommend permanent marks but if you choose not to have them, you will need to take extra care while washing. Don’t try to redraw the marks if they do wear away or smudge. Tell one of the team when you arrive for your next treatment and you’ll be able to have them replaced.
Although you will need to remove some of your clothing, you will be covered up as much as possible and your privacy will be respected. Once you’re lying on the planning bed - part of a specialist piece of equipment called a simulator or scanner - the radiographers will make sure you’re comfortable. This is important, as you will need to maintain that position for both the planning procedure (20-30 minutes) and your radiotherapy treatment. X-rays and measurements will be taken as part of your radiotherapy record during the planning procedure.
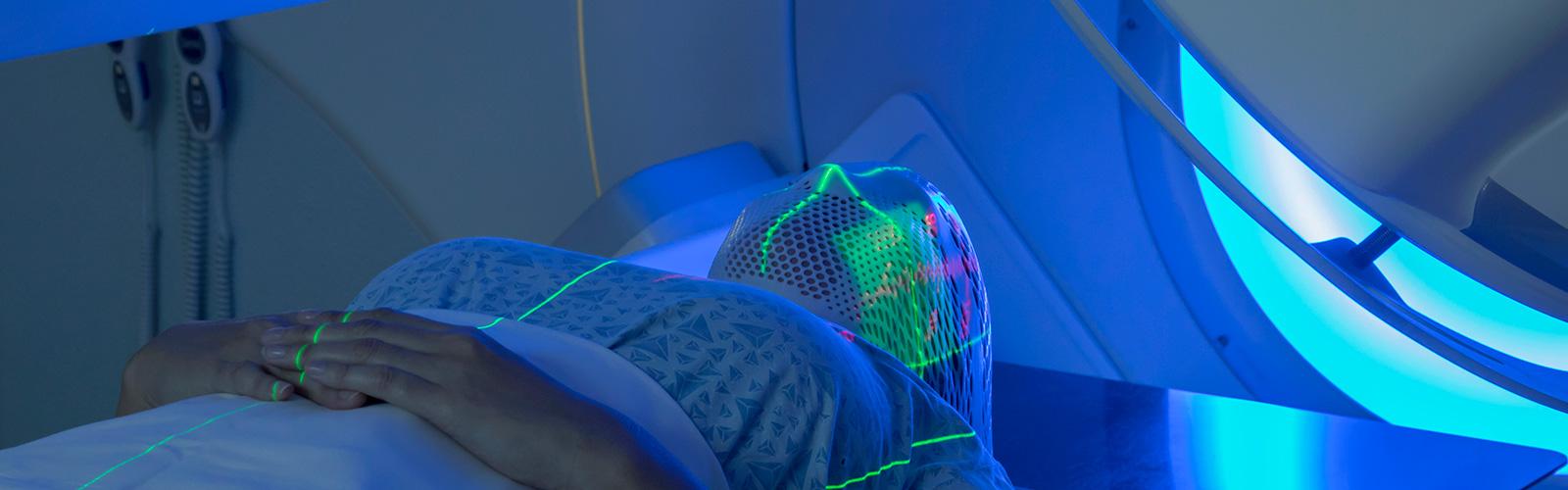
For some treatments, we create a device called a ‘cast’, which is placed onto your body both for planning and treatment. This is most commonly needed for radiotherapy to the head and neck. Its main purpose is to help you to stay still but it also means we can place reference and treatment marks onto the cast rather than your skin.

Treatment
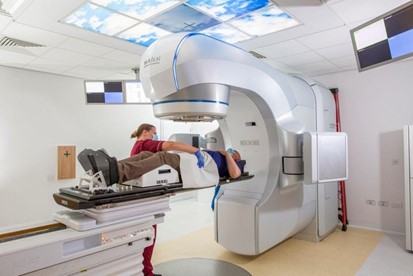
The treatment room - external beam radiotherapy
The treatment procedure is similar to planning and also painless. You will probably be in the room for 10-15 minutes, but delivering the treatment only lasts for a few minutes. The radiographers will discuss any pre-treatment procedures with you each day, such as emptying your bladder,
You will need to remove or loosen your clothing and lie on the treatment couch. We will use some equipment to help you stay comfortable and in the correct position.
The radiographers will align you with the treatment machine according to the details of your treatment map. After the set-up process, they have to leave the room to switch on the machine, which will make a humming or buzzing noise. You should lie still and breathe normally.
Side effects
Side effects are determined by many factors, including the total dose, the number of treatments and the part of the body being treated.
Physical effects are related to the organs included in the treatment field, (e.g. bladder, lungs) and tiredness/fatigue is also common.
Temporary side effects are short-term or acute, and occur while you are attending the department. They may last from a few weeks to several months after treatment. Long-term or permanent effects are quite rare but they do occur. They won’t necessarily be serious and are often easily managed.
Please note that you do not become radioactive as a result of having External Beam Radiotherapy, so there is no danger to anyone else, including children and babies. However, if you need any of the specialised procedures, which use tiny doses of radioactive material, you will be told about the necessary safety precautions.
Radiotherapy and skin care
Most radiotherapy patients are prone to developing temporary skin reactions. Your skin condition will be checked regularly and you’ll be given advice and medication should you need it.
The likelihood and severity of any reaction will be determined by the way the radiation is delivered and the dose received by the skin. Usually, the more treatments you receive, the more likely you are to experience a reaction on some or all of the skin being treated. This is often in the areas where the beam enters and leaves your body.
Changes often start approximately 10-14 days after the first treatment. The skin will become drier, redder and slightly irritated. You may experience a more severe reaction, depending upon the total dose of radiotherapy and the area of your body being treated. The skin will be very red, sore and it may become moist and feel warm.
You will be given appropriate medicines, including painkillers, creams and dressings, to help you cope.
After completing your radiotherapy, you can expect your skin condition to continue and even worsen over the following 10-14 days. The skin will then begin to heal and will recover within a few weeks. Keep using any creams you have been given; they can’t stop the reaction but they will help soothe the skin.
All patients receiving radiotherapy potentially risk developing long-term skin changes, which could include a lighter or more varied colouration of the skin, some reduction in elasticity. and thin, spidery red lines called telangiectasia (this is rare). The long-term risks of skin changes will be discussed as part of the consent procedure. If you are in a higher risk group, the risks will be discussed in more detail.
In practice, the risk is greatly reduced due to the development of new equipment that decreases the dose to the skin.
After treatment
As your radiotherapy comes to an end, you will be given information about what to expect over the next few weeks/months.
A doctor from the Oncology team will see the majority of patients within a few weeks of their final treatment and this appointment is usually at your local hospital.
If you are already under the care of a District or Macmillan Nurse it will be helpful to contact them when you have completed your radiotherapy.
If you have any new nursing needs as a result of your radiotherapy, the staff will discuss this with you and, with your permission, arrange for you to be contacted by appropriate staff such as a District Nurse.
A few days after the completion of your radiotherapy, a short summary is sent to your GP. A formal letter will be sent from a doctor on the Oncology team within a few weeks.
If you need a repeat prescription of any medicines or creams supplied by the Centre, you should make an appointment to see your GP. It may be useful to take an empty box/bottle with the details of the medicine.
Recovery
It can take many months before you feel fully recovered fully and able to do all the things you did before your diagnosis and treatment. If you are feeling low or experiencing mood swings it may be helpful to talk to health care staff or specialist cancer care staff that have been involved in your care.
You may find it useful to talk to others who have experienced cancer by attending a local support group. Contact the Macmillan Information and Support Centre for more details.
Being active
If you have to reduce your activity levels as a result of coping with treatment, make sure you build up the duration and frequency of any activity gradually and at your own pace.
Diet
If you have to modify your diet as a result of receiving radiotherapy, you should try to return to a normal diet as soon as any symptoms have settled. You may want to take the opportunity to consider your diet and include a greater variety of foods to improve or maintain good health.
Leaflets on a healthy diet are available in the Radiotherapy departmen